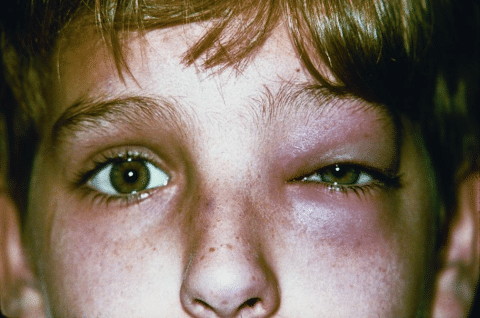
Dr. Ian Boydstun, DO – Northwest Eye Surgeons Seattle
Preseptal and orbital cellulitis represent a spectrum of inflammatory states involving the soft tissues around the eye. The naming scheme is based on the location of affected tissues, preseptal cellulitis being anterior to the orbital septum and orbital cellulitis being posterior to the orbital septum. This distinction also carries clinical significance in that preseptal cellulitis is generally a less severe infection that can often be managed outpatient, whereas orbital cellulitis is a true ophthalmic emergency with the potential for permanent vision loss, intracranial spread, cavernous sinus thrombosis, and systemic complications. The orbital septum acts as an anatomic barrier, but it is not absolute, and infection can move from anterior to posterior structures if not recognized and treated appropriately.
Preseptal Cellulitis
Preseptal cellulitis typically presents with eyelid and periocular edema, erythema, warmth to the touch, and tenderness to palpation. Patients or parents often report rapid onset swelling over 24 to 48 hours. In contrast to orbital cellulitis, visual acuity, pupillary responses and extraocular motility are unaffected. There is no proptosis and there is no pain with extraocular motility. The absence of ophthalmoplegia, diplopia, or vision changes helps localize the infection anterior to the septum and distinguish it from orbital involvement.
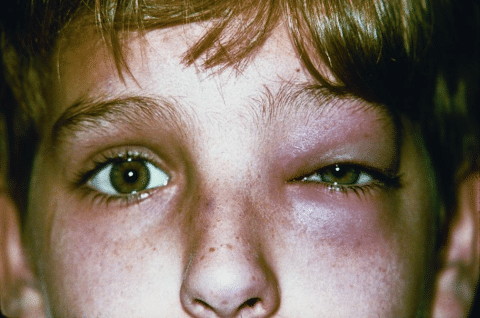
Figure 1: Photograph showing left periorbital edema and erythema seen in preseptal cellulitis.
Children are more commonly affected by preseptal cellulitis than adults, often in the setting of sinusitis or recent upper respiratory infection. In younger children bacteremia can also spread the periocular tissues. In contrast, adults tend to have more localized sources such as cutaneous trauma, insect bites, hordeolum, or dacryocystitis. The microbiology reflects these differences. Staphylococcus aureus and streptococcal species are the most common bacterial causes. Community acquired MRSA should be considered where prevalence is high, as this may affect first line antibiotic choice. In vaccinated pediatric populations Haemophilus influenzae type b is now rare but historically was an important cause of more severe periorbital infections.
Uncomplicated preseptal cellulitis in an otherwise healthy child or adult without systemic symptoms can often be managed with oral broad-spectrum antibiotics that target common Gram-positive species, with MRSA coverage as appropriate. Oral antibiotic options include amoxicillin/clavulanate, first generation or second generation cephalosporins, and clindamycin. Close follow up within 24 to 48 hours is essential to confirm clinical improvement. Lack of improvement should prompt reconsideration of the diagnosis, assessment of adherence, and imaging to exclude orbital involvement.
Special consideration should be given to infants and immunocompromised patients who should be hospitalized for closer monitoring during management, as the clinical course can rapidly change with this population. If there are significant systemic signs or eyelid swelling is so severe that a complete ophthalmic exam cannot be performed to rule out orbital involvement, the patient should be admitted to the hospital and imaging performed to exclude posterior spread. CT imaging of the orbits and sinuses with contrast is typically preferred in the acute setting as it provides rapid assessment of sinus disease and orbital extension. Surgical drainage is rarely needed for preseptal cellulitis and is generally limited to localized abscesses anterior to the septum. When drainage is performed cultures can guide antibiotic refinement.
Orbital Cellulitis
Orbital cellulitis involves infection of the tissues posterior to the orbital septum. This is a true ophthalmic emergency that requires rapid intervention. Most commonly this is due to extension of bacterial sinusitis, particularly the ethmoid sinus in children given the thin lamina papyracea and valveless venous system that allow spread into the orbit. In adults infection may also extend from the frontal or maxillary sinuses, dental infections, facial trauma, or hematogenous spread in the setting of systemic infection.
Clinically orbital cellulitis presents with fever, malaise, chemosis, painful and restricted extraocular movements and varying degrees of proptosis. Eyelid edema can be significant and may resemble preseptal disease at first glance. Diplopia is common due to limitation of extraocular motility. Other signs of optic nerve compromise such as decreased visual acuity, color desaturation, constricted visual fields, and RAPD are more ominous and concerning for optic neuropathy. Elevated intraocular pressure can also be seen due to orbital congestion. These are the clinical signs that differentiate from preseptal localization.
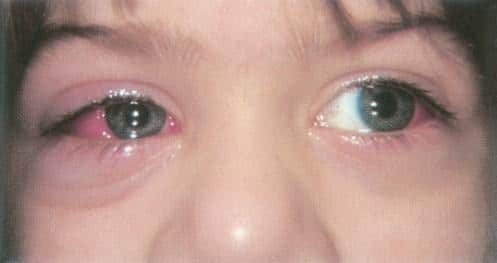
Figure 2: Photograph showing mild right periorbital edema with chemosis, hyperemia, and limitation of extraocular motility in left gaze seen in orbital cellulitis.
Orbital cellulitis requires hospitalization, urgent broad spectrum intravenous antibiotics, and contrast-enhanced CT scan of the orbits and sinuses. MRI may be considered if there is concern for intracranial extension or cavernous sinus involvement. Additional specialists like ENT and/or oculoplastics should be consulted if an orbital abscess is identified or if there is extensive sinus disease requiring surgical management. Early collaboration is especially important in adult patients who more frequently have polymicrobial infections and a higher likelihood of needing operative intervention.
Children are more likely than adults to improve with systemic medication even in the presence of a subperiosteal abscess. Several factors including abscess size, patient age, location of the abscess, and visual findings influence the decision to operate. Emergent drainage is typically reserved for cases with pupillary abnormalities or other signs of optic nerve compromise, large non medial abscesses, worsening ophthalmic findings despite appropriate antibiotics, or lack of clinical improvement after 24 to 48 hours. Proptosis and limited extraocular motility can rapidly improve in children less than 9 years of age due to such a favorable response to IV antibiotics alone.
Common empiric intravenous antibiotic choices include vancomycin combined with a third generation cephalosporin such as ceftriaxone or with ampicillin/sulbactam to provide coverage for MRSA, streptococci, and anaerobes associated with sinus disease. Blood cultures are often obtained in febrile children and cultures from sinus or abscess drainage allow antibiotic choice to be fine tuned once results are available. Repeat imaging may be needed if there is no clinical improvement within 24 to 48 hours, as subperiosteal or true orbital abscesses may require surgical drainage. Duration of therapy typically includes several days of intravenous antibiotics followed by transition to an extended oral course once clear clinical improvement has been seen.
Conclusion
Preseptal and orbital cellulitis require careful clinical distinction to ensure appropriate management. The anatomic boundary of the orbital septum helps to categorize these entities but exam findings and clinical judgment are crucial in determining the true extent of infection. Preseptal cellulitis is generally less severe, often managed outpatient with oral antibiotics and close follow up, especially in older children and adults. Early reassessment is key to ensuring that posterior spread is not missed.
Orbital cellulitis, on the other hand, is a medical and often times surgical emergency requiring hospital-based care, IV broad-spectrum antibiotics, imaging, and a multidisciplinary team. Early recognition of optic nerve compromise and involvement of ENT and oculoplastics can preserve vision and reduce morbidity. The age specific presentations, microbiologic patterns, and expected response to therapy guides a provider’s decision making for children and adults alike. Maintaining a high index of suspicion in young children and immunocompromised patients helps reduce the risk of serious outcomes such as vision loss, intracranial extension, and life threatening complications.
Sources
American Academy of Ophthalmology. Pediatric Ophthalmology and Strabismus. Basic and Clinical Science Course. 2015–2016 ed. San Francisco, CA: American Academy of Ophthalmology; 2015.
American Academy of Ophthalmology. Orbit, Eyelids, and Lacrimal System. Basic and Clinical Science Course. 2015–2016 ed. San Francisco, CA: American Academy of Ophthalmology; 2015.
Brook I. Microbiology and antimicrobial management of orbital cellulitis. Pediatrics. 2007;119(3):e759–e766.
Garcia GH, Harris GJ. Criteria for nonsurgical management of subperiosteal abscess of the orbit in children. Ophthal Plast Reconstr Surg. 2000;16(6):380–386.
Lee S, Yen MT. Management of preseptal and orbital cellulitis. Saudi J Ophthalmol. 2011;25(1):21–29.


